|
Scleral lenses are life changing devices for people with irregular corneas from conditions like keratoconus, corneal transplants, failed LASIK, corneal scarring and dry eye disease. They offer significant improvements in visual acuity and can give patents with these conditions the ability to see and function normally with comfort and consistency. They act as a prosthetic that can be worn during the day to greatly reduce blur, glare, and light sensitivity.
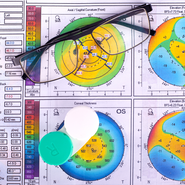
Patients with these conditions suffer from excessive amounts of what are known as higher order aberrations (HOAs). Aberrations exist in virtually every eye. Typical aberrations (lower order aberrations) include myopia (near sightedness), hyperopia (far-sightedness) and astigmatism, can be easily corrected with glasses and soft contact lenses. People with eye diseases like keratoconus have additional higher order aberrations (trefoil, coma, etc) that cause significant blur, glare at night, star-bursting, haloes, and “ghosting” of letters and images. These HOAs cannot be corrected with typical vision correction devices like glasses and soft contact lenses. Rigid lenses like traditional scleral lenses and corneal gas permeable lenses can correct a significant amount of HOAs and greatly improve vision for these individuals, but often there are still residual HOAs that can persist and prevent clarity. Kirkwood Eye Associates is now the first and only practice in Missouri with the ability to detect these residual HOAs with the help of the XWAVE system from OVITZ, and the ability to incorporate the proper correction onto a number of scleral lens platforms. The process involves using the XWAVE aberrometer to measure the amount of HOAs present in an eye wearing a traditional scleral lens. The measurements can then be used to design a wavefront guided optic zone on a scleral lens to further reduce presence of HOAs and improve visual acuity and clarity. This process requires perfect scleral lens stability to properly align the optics to correct these imperfections in the visual system. The scleral lens experts at Kirkwood Eye Associates utilize cutting edge technologies like scleral mapping and impression scleral molding to design lenses with the optimal fit necessary to align these precision optical corrections. It is important to note that likely every human eye has some detectable level of HOAs and it is impossible to get that level to zero with current technology, but the OVITZ software can often help people with corneal disease bring their HOAs to a level at or below what we would expect in a non-diseased eye. HOA correction is not currently covered by any vision or medical insurance. If you do have a plan with “medically necessary” coverage, please note that HOA correction will still be an out-of-pocket add-on feature. Contact Kirkwood Eye Associates today to see if HOA-correcting scleral lenses can help improve your vision.
0 Comments
Valued Patients,
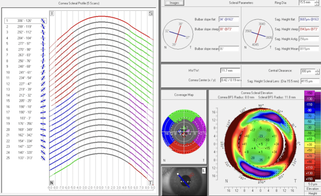
At Kirkwood Eye Associates, our goal is to deliver exceptionally personal patient care in a welcoming setting. Continuing with this tradition, we are excited to announce we are expanding our practice with a second location in downtown Eureka, MO. We have acquired the practice of Dr. Gregory Boschert who has practiced in St. Louis for nearly 50 years. The practice, now known as Eureka Eye Care, sits right along the very same railroad tracks that run in front of our Kirkwood office, symbolically connecting the two practices. You'll find the same friendly care and much of the same technology that makes the experience in Kirkwood so efficient and unique. Please note that all scleral lens, keratoconus, and ortho-k patients will be serviced exclusively in Kirkwood at this time. With a second doctor on our team, we will be able to expand our weekday hours at Kirkwood Eye Associates to better meet your needs. I will see patients in Kirkwood Monday through Thursday. A new doctor will be joining our staff to take over in Kirkwood on Fridays. Eureka Eye Care hours are available Monday, Tuesday, Thursday, and Friday. Please feel free to reach out to us with any questions or concerns. Thank you for trusting your vision care to us and we will work every day to exceed your expectations. As always, thanks for supporting local. Sincerely, Dr. Biondo Scleral lenses are life changing devices for a wide variety of patients. These custom devices help give crisp vision to people suffering from keratoconus, post-LASIK, corneal transplant, corneal scarring, high astigmatism and much more. They are extremely comfortable, stable, and easy to wear. They also offer relief from severe dry eye syndrome. This relatively new technology continues to evolve at a rapid pace and there are new options that utilize technology to improve fit, comfort and vision. These options range from: good (diagnostic fit), to better (custom scan fit,) to best (impression mold design). Diagnostic Fitting (Good) This is the traditional method for fitting scleral lenses. Diagnostic (trial) lenses are placed on the eye in the office to determine the best fit and power for the patients eye. These designs continue to improve and are becoming more customizable each year, but still have limitations on how “fine-tuned” the fit can be based on manufacturer specifications. Custom Scan Fitting (Better) Thanks to a new piece of equipment here at Kirkwood Eye know as the Pentacam Corneo-Scleral Profiler, we can now scan the entire front surface of the eye including the cornea and surrounding sclera (the white part of the eye). Traditional topographers only measure the cornea. This is important because scleral lenses rest completely on the sclera. This technology allows us to scan the scleral topography (shape) and custom design a lens to match the unique curvature of each patients eye for an exacting fit in all meridians. This not only improves comfort and vision, it also reduces the need for remakes and additional office visits to “fine-tune” the design. Impression Molded Design (Best) This technique is similar to the process used for a dental mold. A bio-compatible compound is loaded in to a tray and placed against the ocular surface for about 90 seconds. There is no pain and it feels similar to wearing a contact lens. The compound hardens and is gently removed, leaving a perfect impression of the surface of the eye. The impressions are sent to a lab where scleral lenses are designed in a 3D environment to perfectly match the patient eye down to 2 microns of tolerance (a micron is one millionth of a meter). This design is great for anyone looking for a perfect fit from day one and is especially useful for people with scleral irregularities like glaucoma shunts or other elevations.  Orthokeratology (also know as ortho-k or corneal reshaping) is a safe and effective overnight treatment for myopia, or “near-sightedness.” Myopia, or near-sightedness, is on the rise in a big way. Not only are more children than ever developing myopia, the severity is also increasing rapidly. The prevalence of myopia has increased 66% in this country since 1971 and it’s estimated that half of the world's population will be myopic by 2050. Higher levels of myopia have a number of negative health consequences. Risks include an increase likelihood of glaucoma, early cataracts, and retinal detachments. Higher amounts of myopia also impact quality of life as they result in and increase dependency in vision correction devices and a reduction in refractive surgery candidacy. How does orthokeratology work? Orthokeratology (ortho-k) is a process that involves wearing an overnight contact lens device. The device gently molds the cornea to correct myopia and thereby eliminates the need for any daytime contacts or glasses. The treatment also help to stop or significantly slow the progression of myopia, making it ideal for children and teenagers. The treatment effects are reversible by simply discontinuing the devices. Is orthokeratology safe? Ortho-k was FDA approved in 2001 and is a safe and effective treatment for myopia. It’s myopia control effect makes it far more beneficial for younger patients than traditional contacts and glasses. The risks associated with orthokeratology are the same as those for any contact lens wearer and can be mitigated with proper lens hygiene. Who should have ortho-k? Anyone with a prescription under -5.00D and with minimal astigmatism is a good candidate for orthokeratology, but it is especially beneficial for children and people under 21 years old, since they will have the highest risk of myopic progression with traditional contacts and glasses. There is no minimum age under the FDA approval, and we at Kirkwood Eye Associates have successfully treated patients as young as 6 years old. The earlier you start ortho-k, the better you can control the myopia. Typically, we offer to move patients into traditional vision correction devices or consider refractive surgery after 21 years of age, but some patients elect to continue ortho-k through their 20’s and beyond because of its convince. How much does ortho-k cost? Is it covered by insurance? Cost can vary depending on the extent of treatment but it typically is around $80 a month. Some more advance and high risk patients might require atropine therapy that can slightly increase the fee. The treatment is not covered by vision or medical insurance. Are there alternatives to ortho-k? There are other myopia control options offered at Kirkwood Eye Associates. Atropine drop therapy is a compounded medication that can help slow eye growth. MiSight soft daily disposable soft contact lenses are FDA approved to slow down myopic progression as well.
Keratoconus is a progressive corneal disease that effects roughly 1 in 2000 Americans according to the national institute of health. It causes blurred vision that may not be correctable with standard spectacles or soft contact lenses. Other symptoms can include glare, haloes, and rarely, pain. Keratoconus is not an inherently blinding condition, but in its severe forms it can result in the need for a corneal transplant. Scleral lenses offer keratoconic patients significant visual rehabilitation and are comfortable and stable. They can be successful for nearly any patient, even those who have failed other contact lenses in the past like corneal gas permeable lenses and hybrid lenses. They are also shown to reduce or alleviate the need for a corneal transplant.
Dry eye disease patients can do exceptionally well with scleral lenses. Because these devices hold a layer of moisturizing tears against he ocular surface all day, they can offer relief from dry eye symptoms and improved quality of life. Many studies highlight the reduction or discontinuation of the need for eye drops and medications, as well as improved visual acuity and visual stability. Post corneal surgery patients (LASIK, Corneal Transplant, RK, PRK) can be left with corneal surface irregularities that prevent them from seeing as crisply as they would like, especially at night. These irregularities cannot be corrected with spectacles, soft contact lenses or other surgeries. Scleral lenses can give back the crisp 20/20 vision that allows you to see clearly at night or follow a golf ball off of the tee. At Kirkwood Eye Associates, we have invested in the latest technology to fit scleral lenses. We are one of the only practices in the state to offer Eyeprint custom molded scleral lenses that accurately match the ocular surface down to 2 microns. We are one of the first to have a machine that utilizes complete scleral surface mapping to design lenses that are accurate down to 10 microns. Both of these options far exceed the ability to fit with diagnostic lenses alone. Call today to see if scleral lenses can change your life.
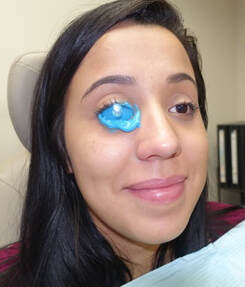
Attention scleral lens wearers! We at Kirkwood Eye Associates are proud to be national leaders in scleral lens fitting for dry eye, keratoconus, and irregular cornea patients. We are excited to announce the addition of the EyePrint Pro Scleral Device System to our practice. This highly customized scleral lens fitting utilizes a compound that is inserted onto the surface of the eye and makes an impression of the globe. That impression is 3D analyzed and a perfectly molded scleral device is produced for your eye.
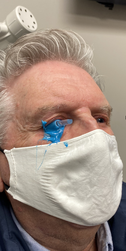
We at Kirkwood Eye Associates are excited to offer the next generation tool in the fight against dry eye disease. We are the first practice in St. Louis to offer Low Level Laser Therapy (LLLT) to treat meibomian gland dysfunction (MGD) and dry eye diseases (DED). This revolutionary treatment is done in office and is safe, painless and effective in unclogging tear glands and up regulating tear production to allow for a more stabile and robust tear film. We have always strived to offer the latest in-office therapies to treat dry eye including the Lipiflow, the iLux, the ABmax Blepharo-exfoliator, punctal occlusion, amniotic membrane therapy, demodex treaments and more. In-office dry eye treatments have many advantages over at-home therapies and prescription drugs. They often cost less over time, have little or no side effects, don’t require nightly care regimens and, best of all, they target the cause of the tear film dysfunction and allow the eye to work for itself, instead of relying on prescription drugs. How does LLLT work? Simply put, a mask is placed over the eyes and upper face that is equipped with high energy diodes that emit a specific wavelength of light. This up-regulates the action of the cells powerhouse known as mitochondria. This achieves two results. First, this increased metabolic activity inside the tear glands generates heat that melts blockages in the meibomian glands and lacrimal glands, allowing tears to flow more freely. Second, the increase in metabolism charges the tear glands, increasing tear output. Added bonus… this treatment also boosts collagen production around the eye area and can help alleviate wrinkles. The result is clear and robust lipid and aqueous production, the two building blocks of our tear film. The treatment lasts 15 minutes and is painless. I can be repeated as often as necessary to alleviate symptoms and keep them at bay. We often combine this therapy with eyelash exfoliation to clear away dirt, bacteria and biofilm from the lid margin that can clog and disrupt gland function. For more severe cases, it can also be combined with the iLux meibomian gland expression system. This brand new technology is FDA approved and has been used for years in Europe with great success. It is not covered by insurance but treatments often cost less than a month of dry eye medications like Xiidra or Restasis and don’t require daily drop instillation that sting and bad taste. Conditions that would benefit from LLLT: Dry Eye and meibomian gland dysfunction (MGD) Chalazion Ocular Rosacea Demodex Blepharitis Post-Blepharoplasty If you have dry eye of any severity, from mild contact lens dryness to stinging eyes at the computer, to severe painful dry eye secondary to an autoimmune condition, call us to set up an appointment for this exciting new treatment. As the Coronavirus pandemic continues, patients continue top ask about aspects of their health pertaining to their every day life, including contact lens wear. When it comes to contact lens wear, the American Optometric Association (AOA) and the Center For Disease Control (CDC) both state that contact lenses are still a safe and contact lens wearers shows no greater risk from COVID-19 than those wearing glasses. Here are some pointers and myth-busters to guide you through the outbreak. Contact lenses themselves will not give you COVID 19. Proper hygiene is always important when handling contact lenses, and this is even more important than ever because of the need to touch your face and eyes. Be sure to wash your hand thoroughly! Exercise proper hand washing technique. The CDC recommends at least 20 seconds of hand washing, followed by hand drying with unused paper towels. This should occur before every contact lens insertion and removal. If soap and water are unavailable, use a hand sanitizer that contains at least 60% alcohol. This is less ideal because residual alcohol can cause mild sting and temporary irritation, but it's still better than not sanitizing hands at all. Routinely disinfect contact lenses. If you are in a single use (daily disposable) contact, be sure to discard at the end of each wear. If you are in a reusable contact lens make sure to follow the manufacturer recommended care regimen. If you do get sick, discontinue lens wear. Contact lenses should never be worn if your have an acute illness like a cold or the flu. If you experience flu-like symptoms, discontinue contact lens wear and stick to glasses. Glasses are not proven to offer protection. Glasses and contacts carry the same risk because they both require face touching. Proper hygiene will allow either modality to be utilized safely. If you have a contact lens prescription that is nearing expiration or has expired, call our office at 314.394.3045. We are working with our patients to ensure you have access to lenses as needed. We are also accepting appointments, but no walk - ins at this time. No federal laws related to the Contact Lens Rule prescription verification process have been suspended or waived. We continue to be here for you and your eye care needs throughout the "Stay at Home Order" in Saint Louis city and county. To learn more about the extra precautions we are taking, click below. Individuals should continue to consult the Centers for Disease Control and Prevention guidance on how to protect themselves from COVID-19.
It’s no secret that most of us spend too much time in front of a screen. Many people spend all day at work staring at a computer monitor, only to come home and spend hours on a phone or tablet. This kind of extended near work takes a toll on our tear film, the protective layer of hydration on the surface of our eye. Our pre-corneal tear film is an extremely complex and important component of our visual system. It protects our sensitive ocular surface from the environment and any disruption in this layer leads to symptoms ranging from tired eyes to burning, tearing and itching. The tear layer also serves a very important optical function. The surface of our eye is rough and uneven… not ideal for focusing light precisely on the retina. Our pre-corneal tear film fills in these irregularities and creates a smooth and uniform surface for refraction. This is the reason that the majority of dry eye sufferers present with complaints of blurred and variable vision, not eyes that feel dry or uncomfortable. So why does screen time lead to tear film instability and dry eye? This mainly is due to our lack of full and complete blinks while focusing on our near work. Any extended near focusing (even a book) causes us to blink one-third as much as we normally would, but screens make it even worse. Images on digital devices change and refresh so quickly, we not only blink less, we have incomplete blinks because. A full and complete blink may mean that we miss something on our facebook timeline!
This issue is that a lack of blinking (and complete blinking) leads to blocked up tear glands. Our eyelids contain glands that make up two of the three layers of our tear film. Accessory lacrimal glands secrete the watery part of our tears and (most importantly) meibomian glands secret oils that cover and protect our tears, holding the system together between blinks. In order for these glands to properly express their contents, one must achieve a full blink that causes small muscles around the glands to contract, expressing their contents. When we chronically fail to do this, the oils and tears start to coagulate in the glands and lead to blockages, causing dry eye. Another cause of dry eye symptoms (blurred vision included) is an accumulation of microorganisms along the eyelash line (blepharitis). These can include bacteria (mainly the staph that typically inhabits our skin surface) and parasites like the demodex mite. Our lashes provide the shelter, oils and moisture to promote microbial growth. Combine that with the fact that most people fail to wash their lashes on a daily basis and you have a recipe for infestation. These microorganisms do more that just gross us out… they release exotoxins, oil destructive enzymes and other byproducts that irritate our ocular surface and inflame our eyelid margins. They can even cause more direct damage by infesting our glands leading to improper tear production and styes. If you suffer from chronic styes, we can help! So what can be done? If you are not experiencing any symptoms, its still worth getting check out. Early detection of lid disease through examination and gland imaging is paramount in preventing dry eye symptoms. This is also the best time to begin lid hygiene with doctor recommended lid scrubs to prevent blockages and infestations. It is also important to remember to take frequent breaks from digital device and BLINK!! If you’re already experiencing ocular fatigue, discomfort or blurred/variable vision, it may be time to consider in-office treatment. These treatments can be tailored to treat your specific lid disease. Treatments often include blepharo-exfoliation that removes dirt, metabolic debris, bacteria and parasites from the eyelid margin. This helps allow the tear producing glands in the lids to function optimally. Additionally, meibomian gland expression ( iLux ) is a new and extremely effective method of instantly and painlessly improving tear quality and reducing dry eye symptoms through the unclogging of blocked glands. These treatments have shown a success rate of over 85% in our practice. While treatment like these are not covered by insurance, they are far more effective than over-the-counter or prescription eye drops and tend to be far cheaper when extrapolated over a years time. At Kirkwood Eye Associates, we remain committed to being at the forefront of dry eye therapy, most of which is now done in the office, reducing or removing the need for daily home therapy that is less effective and more time consuming (and typically more expensive). In office treatments include blepharo-exfoliation, iLux meibomian gland expression (replacing lipiflow), amniotic membrane therapy, punctal plugs, bandage contact lenses and more. Call us today if you’re tired of tired eyes!
The Skin Cancer Foundation's Seal of Recommendation is granted to sun protection products that have been reviewed by and meet the specific criteria of an independent Photobiology Committee (experts in the study of the interaction of ultraviolet light and the skin). In order for sunglasses to earn the Seal of Recommendation, they must filter out at least 99 percent of ultraviolet A (UVA) and ultraviolet B (UVB) radiation.
"The Seal of Recommendation is a symbol of safe and effective sun protection that is recognized by consumers worldwide," said Perry Robins, MD, President of The Skin Cancer Foundation. "One of the first programs offered by the Foundation, it quickly gained acceptance from consumers for setting the standard for effective sun protection. Maui Jim received our Seal because all of their sunglasses exceed our requirements and protect against 100 percent of UVA and UVB rays." All Maui Jim sunglasses are able to meet the stringent requirements of The Skin Cancer Foundation because the company's PolarizedPlus2® lens technology uses up to nine layers of protection on both sides of each lens to eliminate 100 percent of UVA and UVB rays and 99.9 percent of glare from above, below and behind each lens. Maui Jim lenses block 100% of all harmful UV rays, protecting your eyes from damage and long-term health risks. Sunglasses that do not provide UV protection can actually cause more damage because they shade the eye, allowing for more UV rays to hit the pupil. Another reason these lenses are top of the line? Blue-Light protection. High-energy Visible Radiation (HEV), also known as blue light, has lower energy rays than UV, however recent research suggests they can penetrate the eye and cause damage. Maui Jim patented lens technology, provides HEV reduction without removing the blues. Maui Jim sunglasses won't change the world, but they'll change the way you see it; vivid colors, improved clarity, and crisp details—all while blocking glare and harmful UV. |
AuthorAndrew Biondo, OD, FSLS is the Primary Medical Director at Kirkwood Eye Associates in Kirkwood, MO. Serving the greater St. Louis area, Dr. Biondo has 12 years of experience as an eye care provider, health educator & consultant to the specialty contact lens industry. His special interests include contact lenses, dry eye disease, glaucoma, macular degeneration, laser eye surgery & preventive vision care. Archives
May 2024
Categories |
Contact us:
|
Location:
|
Stay in the loop!
|











 RSS Feed
RSS Feed